Human milk–based fortifiers matter to critically ill and premature infants
Premature infants need additional calories and protein that are vital to their survival, growth, and development.
While breastmilk is perfect nutrition for babies, it does not provide enough nutrition for preemies.
For preterm infants the American Academy of Pediatrics (AAP) recommends adding a “human milk fortifier” to mother’s own milk or pasteurized donor breastmilk for babies born weighing 3.3 pounds (1500 grams) or less.1 These fortifiers provide the added calories and protein preemies need.
Term babies recovering from surgery repairing gastroschisis may also need nutritional support including fortifiers. In 2025, the US Food and Drug Administration approved the first human milk-based fortifier for use in term infants with Gastroschisis following surgical repair. Learn more

Understanding your nutrition options in the NICU will help you and your care team make the right choice for your baby.
Human milk = vital nutrition to thrive
Breastmilk plays a vital role in your preterm baby’s health. When your care team adds Prolacta’s fortifiers, the goal is to achieve improved health outcomes as shown in clinical studies.2,3,4,5,6,7 These can include decreases in:
- Bronchopulmonary dysplasia (BPD)5,6,8
- Late-onset sepsis5,7 and evaluations8
- Retinopathy of prematurity (ROP)5,6,8
- Necrotizing enterocolitis (NEC)2,5
- Feeding intolerance decreases6
Studies have also shown that premature infants can go home sooner from the NICU with the use of Prolacta’s fortifiers.5,6
Not all “human milk fortifiers” are made from human milk
There are two types of fortifiers available in the hospital. While both are labeled “human milk fortifier,” one type is made from cow milk.
Studies have shown cow milk-based fortifiers can trigger feeding intolerance and increase mortality due to the risk of severe complications. These complications can include late-onset sepsis, bronchopulmonary dysplasia (BPD), retinopathy of prematurity (ROP), and necrotizing enterocolitis (NEC). 2, 3, 4, 6
The other type of human milk fortifiers are made from 100% human milk by Prolacta. The breastmilk used to create our fortifiers is donated by healthy donors. As a part of our extensive screening process, we do a DNA match to ensure all the milk received comes directly from our carefully screened and vetted donors.
It’s important to know your human milk fortifier options. Be sure to talk with your care team about Prolacta’s 100% human milk–based fortifiers.
Helping 125,000+ infants globally, and counting
In clinical studies, preemies weighing 2 pounds 12 ounces (1250 grams) or less at birth fed Prolacta’s fortifiers as part of a 100% human milk diet experienced fewer complications, went home from the hospital sooner, and showed improved growth rates.9,10
In a case series of term infants recovering from gastroschisis repair who received Prolacta's fortifier, Surgifort, improvements in growth velocity and reduced time to full feeds were observed. 11
More than 125,000 critically ill and premature infants globally have benefited from the clinically proven advantages of Prolacta’s human milk–based human milk fortifiers.12
Parent experiences
In addition to the studies, hear from NICU parents who have been where you are now.
Royal Hospital Parent Experience
Disclaimer: This website does not provide medical advice. The information, including but not limited to multimedia content (“Video Content”), contained on this website is for informational purposes only. Video Content represents the views and opinions of the individuals presented and does not necessarily represent the views or opinions of Prolacta Bioscience, Inc. (“Prolacta”). The appearance of Video Content on the site does not constitute an endorsement by Prolacta. No material on this site is intended to be a substitute for professional medical advice. Always seek the advice of your physician or other qualified health care provider with any questions you may have.
When Amy gave birth to her twin boys, Austin and James, at just 24 weeks and 2 days, she faced the uncertainty and challenges that come with an extremely preterm birth. Austin, weighing 650 grams, and James, at 765 grams, needed the best possible nutrition to give them the best possible start.
In the past, NICUs supplemented preemie’s diets with a cow milk-based fortifier. However, at the Royal Hospital for Women, they are using the latest development in NICU nutrition— 100% human milk-based fortifiers mixed with Mother’s Own Milk or donor milk.
Watch the video to hear Amy’s experience and see how human milk is making a difference for NICU babies like Austin and James.
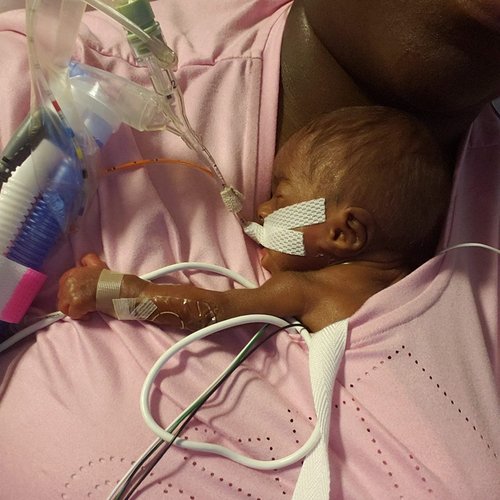
The story of Kallie, as told by her mom, Ebonie
My pregnancy with Kallie was identified as high risk early due to my high blood pressure. My obstetrician proactively managed it and placed me on medication. I didn't gain weight during the pregnancy, as a matter of fact, I lost weight. However, the doctor did not seem too concerned since I was a little overweight to begin with. On May 20, at just 24 weeks and 3 days into my pregnancy, the ultrasound technician noticed several things that were a cause for major concern:
- I lost most of my amniotic fluid
- Kallie was the size of a 21-week-gestation baby even though I was over 24 weeks along
- Blood flow between the placenta to the umbilical cord to Kallie was absent end-diastolic flow
That same day, I was sent to a hospital 40 minutes away and put on bed rest so doctors could closely monitor the blood flow from my placenta and to ensure Kallie stayed inside as a long as possible. At 25 weeks, during a routine umbilical cord ultrasound, the doctors saw that the blood flow to my placenta had started to reverse. It was time for Kallie to be delivered. She was born at 25 weeks gestation via emergency c-section on May 24. She weighed 370 g (13.1 oz) and was whisked away to the hospital's level III neonatal intensive care unit (NICU).
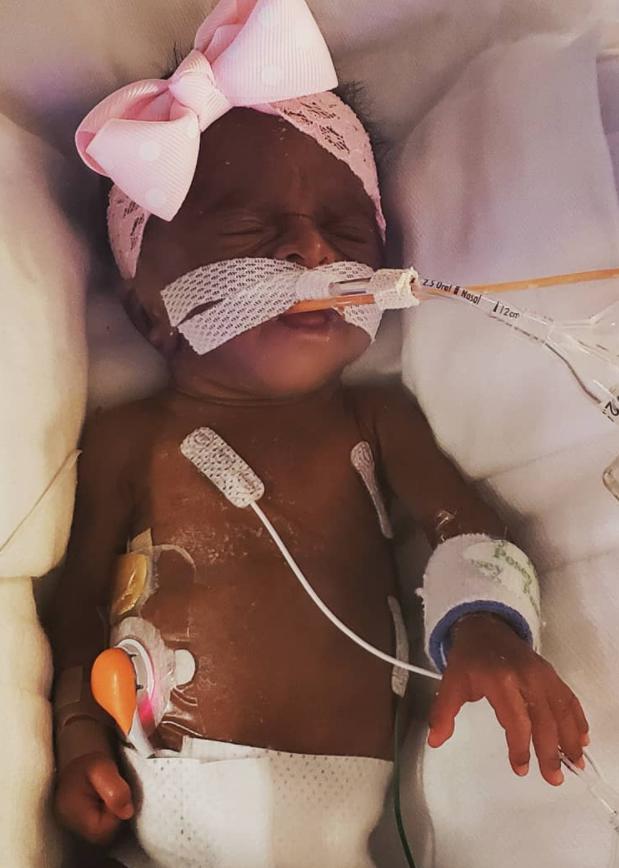
Almost 6 hours after delivery, after most of the medications had worn off, I was wheeled over in my hospital bed to see Kallie for the first time. I had so many feelings and emotions going through my mind at first sight of her. She was smaller than any other baby I had ever seen. I was scared, but I knew she was here for a reason and was ready to fight.
The days in the NICU were long, anxiety was high, and each milestone felt like they took forever to reach. But overall, I would say our NICU experience was good. Kallie needed several blood transfusions, she had one or two bouts of low white blood cell count, and she underwent patent ductus arteriosus (PDA) ligation surgery at 4 weeks old. Our biggest hurdle was oxygen. Kallie was intubated for 8 weeks, and after extubating, she required various forms of ventilation support during her 150-day NICU journey.
Providing breastmilk in the NICU
I started pumping the day Kallie was born and kept pumping every 3 hours. I had ample supply and packed the NICU freezer. Her very first taste of my breastmilk was on a swab through what I learned was called "oral care." Feeding has proven to be our biggest challenge during and after NICU life.
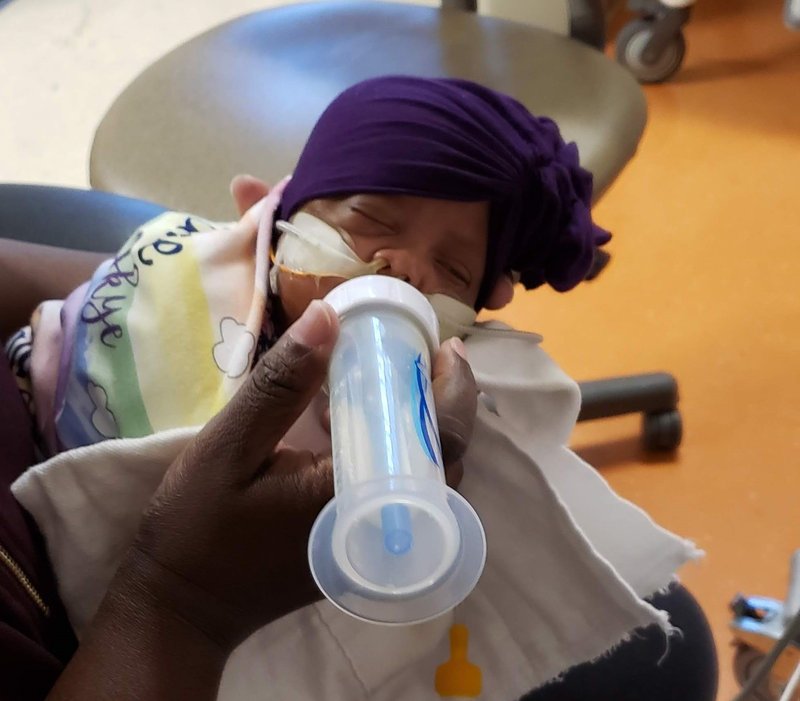
Fortifying my breastmilk
I heard about Prolact+ H2MF from Kallie's neonatologist. She mentioned that Prolacta’s fortifier is made from 100% human milk and it would be added to my breastmilk so that Kallie would get the additional calories she needed to grow and gain weight. Kallie’s first time having Prolacta fortifiers was around 31 weeks gestation for a little less than a month. At the start, she weighed 880 g and one month later she weighed 1435 g, a weight increase of 555 g. The month before getting Prolacta fortifiers, Kallie's weight went from 620 g to 880 g, a weight increase of only 260 g. Looking back, Prolacta fortifiers gave her a great boost and helped her gain more than double the weight she gained the month before. Kallie was extubated 9 days after starting on Prolacta fortifiers.

NICU graduation
Kallie graduated from the NICU at 150 days, just shy of 5 months. She weighed 7 lb 4 oz. She came home with a nasogastric (NG) tube and nasal canula for oxygen support, but all her other milestones were met. Kallie was recognized as one of the smallest babies to ever be cared for at her NICU and made national news.
Advice for parents in the NICU
No matter how long your stay is in the NICU, it’s a hard place to be, but there are so many resources to help you get through it. Join a Facebook group for NICU parents and attend NICU events put on by your hospital. Surrounding yourself with people who are currently in the NICU or who have graduated is the best soup for your soul. They are the ones who will understand your heartaches, pains, and joys. NICU parents celebrate EVERYTHING from moving up in diaper sizes to gaining an OUNCE. Always ask questions and advocate for your baby! And since no two journeys are the same, never ever compare. I hold a special place in my heart for NICU parents.
The story of Evelyne, as told by her mom, Tiffany
"Evelyne is our first baby. Prior to her birth, I had several miscarriages. My pregnancy with Evelyne was not easy—I experienced many complications starting with a hematoma in my early months, followed by an incompetent cervix at 19 weeks which required transportation to another hospital and a rescue cerclage (surgical stitch of the cervix to prevent premature labor). After weeks of bedrest, my water broke at 24 weeks and I was admitted to the hospital on bedrest. Four weeks later, Evelyne was delivered via emergency c-section at 28 weeks gestation weighing 2 lb 8 oz (1130 g)."
The NICU Experience
"My husband and I are vegan and are adamant about living a chemical-free lifestyle. Given this, we really felt it was important to minimize our daughter’s exposure to unnecessary chemicals during her NICU stay. We asked the NICU staff to use chemical-free soaps, lotions, and creams that we brought in and the staff obliged our requests.
Evelyne was on respiratory support until she was 35 weeks and had jaundice but was otherwise healthy under the circumstances. She also had frequent apneas, which were closely monitored and required manual intervention."
Feeding in the NICU
"The same day Evelyne was born I met with a lactation consultant who told me about Prolacta’s 100% human milk–based fortifiers. Prolacta’s fortifiers were available at Evelyne’s NICU, but only for the sickest preemies.
Since Evelyne did not qualify she would be receiving a fortifier made from cow’s milk. As a vegan, we were opposed to this. I insisted that if the NICU felt that a fortifier was necessary for my baby I would refuse anything other than a human milk–based fortifier. Our request moved up the hospital chain of command and eventually we were granted permission to feed Evelyne Prolact+ H2MF® human milk fortifier, the only fortifier made from 100% breastmilk. It was a long process but completely worth it."
After the NICU
"Evelyne was discharged after 81 days in the NICU and weighed about 4 and a half pounds. She is currently 1 year old and thriving, but still quite small weighing only 15 pounds. Her doctor said that she excels in her fine motor skills and was impressed that she could walk with assistance at 10 months of age (6 months corrected). She is a bright and alert baby, with no developmental shortcomings for her actual age. She is truly the happiest baby. My husband and I always tell people she has two moods: happy and sleepy! I credit her current health and vitality to breastmilk, kangaroo care, and Prolacta!"
Advice for NICU Parents
"Be an advocate for your baby and follow your instincts! We were polite but firm with the staff. We listened to their recommendations and did our own research. I know that I did everything in my power and control to ensure that my baby had the healthiest start in life. Speak your mind and advocate for YOUR baby!"
The story of Tommy, as told by his Mom, Sarah
"Tommy was born at 22 weeks and 3 days – 1 day after his brother Timothy’s angelversary. We aren’t sure of Tommy’s exact birth weight because as soon as he came into this world, he was hooked up to medical equipment, but his birth certificate lists it as being 1 lb 5 oz. Tommy was born so early that his eyelids were fused shut, and it was nearly two weeks before he could open them. His veins were so fragile and tiny that it took nurses three tries to get his PICC line in."
NICU Nutrition
"At 24 weeks gestation, Tommy began to receive Prolact+ H2MF fortifier, the only 100% human milk-based human milk fortifier for babies born weighing <1250 grams. All other fortifiers are made from cow’s milk. I am grateful that Prolacta was offered in our neonatal intensive care unit (NICU). But this wasn’t always the case. The story of how Prolacta made its way to our NICU goes like this: A vegan mom refused to have her baby receive a cow milk-based fortifier. She pushed the medical staff to order Prolacta’s fortifier, and through her dogged determination and relentlessness, her preemie was able to receive a 100% human milk diet. The medical staff noticed how well her baby was doing on Prolacta’s product, and the NICU decided to make the switch and offer Polacta’s fortifier to all babies born weighing <1250 grams.
I wanted to make sure Tommy received a diet consisting entirely of human milk in his first few months of life, so I pumped. Pumping was exhausting! With my first child, who was born full term, I had difficulty maintaining a good supply and had to supplement my breast milk with formula for the first 6 months, until we transitioned to 100% formula. Fortunately, with Tommy I was able to pump breast milk for 3 months! He got several infections during his NICU stay, but luckily they were caught in time and responded to antibiotics. At 38 weeks, Tommy had laser surgery for retinopathy of prematurity. Miraculously, he had no brain bleeds, which can be common among 22 weekers. Tommy spent a total of 140 days in the NICU, with 84 of those days being intubated."
After the NICU
"Tommy was discharged from the NICU on oxygen, and after a month home was able to breathe on his own. Today, Tommy is 7 months old (3 months adjusted) and weighs a chunky 11 lb 8 oz! He is able to follow the sounds and lights generated by his toys and is just beginning to develop his fine motor skills. He is like any other baby, making cooing sounds and funny faces and laughing with his big sister, Ellie."
Advice to NICU Parents
- "Advocate for your baby. Speak up for your baby even if it makes you uncomfortable.
- Your nurses will become your biggest support throughout this time, so be nice to them! They're doing their best.
- Make every effort to pump, but don’t let others make you feel guilty if it doesn’t work out for you. Remember, there is always the option of donor milk!
- Connect and find other NICU moms! They will be your biggest cheerleaders and support system.
- Share your baby’s story. By sharing your story as it unfolds, you can be a support and a comfort to someone else going through a similar experience."
What to expect in the NICU
You didn’t plan on your baby spending weeks or even months in the NICU. Learn what to expect in the NICU with your baby.
